Marc Biarnés defends his Doctoral Thesis about the risk factors for the progression of geographic atrophy
02/07/2014 ·
Marc Biarnés has a degree in optics and optometry from the Terrassa University School of Optics and Optometry. He holds a Master’s Degree in public health and a Doctorate in Biomedicine from the Pompeu Fabra University. On 3 July, he defended his Doctoral Thesis Increased fundus autofluorescence, a biomarker of lipofuscin content, as a risk factor for the progression of geographic atrophy secondary to age-related macular degeneration.
Please describe the subject matter and aim of your Doctoral Thesis
The Thesis is based on a prospective longitudinal clinical study that aims to identify the risk factors associated with Geographic Atrophy (GA), an advanced variant of age-related macular degeneration. We were particularly interested in appraising the role played by the increase in autofluorescence, a biomarker of the presence of lipofuscin, a presumably toxic compound. In addition, we attempted to simplify the complex classification of the self-sufficiency patterns of the fundus of the eye, which are interpreted as phenotypes (intrinsic characteristics of each patient) of the disease.
If you were to make a summary, what would this be?
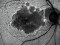
GA is characterised by the presence of areas of atrophy of the pigmentary epithelium of the retina (PER), which grow progressively, with the secondary loss of adjacent photoreceptors and the choriocapillaris. At present, this is an untreatable condition.
The accumulation of lipofuscin in the PER, which is visible clinically through the autofluorescence of the fundus of the eye (AFU) as areas of high autofluorescence, has been linked to the progression of GA in some studies. In fact, certain patterns (“phenotypes”) have been described in the AFU based on the distribution of hyperfluorescence that have been associated with specific progression rates of the disease.
What conclusions has your Doctoral Thesis reached?
Up to now, lipofuscin has been thought to be the determinant in the progression of the disease. By monitoring patients through AFU, which enables identification of the distribution of the lipofuscin in the fundus of the eye, we have determined that this has a more moderate influence than we previously believed.
The most relevant variable was the area of basal atrophy. Large lesions tend to grow faster than smaller ones. That is, there is something in the area of atrophy that determines the progression of the disease. Our impression is that this indicates the perimeter of the lesion to be important and that the perimeter indicates the number of diseased cells of the PER that are in contact with healthy cells.
So now, what is the way forward?
One of the next steps will be to investigate what are the exact causes of transmission of the disease. One of our hypotheses is that the disease grows through some aberrant product transmitted from the diseased cells to healthy cells, as has been observed recently in other neurodegenerative diseases like Alzheimer’s and Parkinson’s. It would be interesting to have tools that enable us to measure the perimeter of lesions in order to validate our hypothesis.